What is Deep Vein Thrombosis?
Deep vein thrombosis (also referred to as DVT, thromboembolism, or venous thrombosis) is a potentially very serious medical issue which occurs when a blood clot becomes lodged in one of the deep veins of the body. This usually occurs in the lower body – either the lower legs, thighs, or pelvis – but clots can also become lodged in the deep veins of the arms, abdominal region, or brain.
What causes DVT?
Anything which unnaturally impedes or slows blood flow can lead to blood pooling in the veins, which causes deep vein thrombosis. There are a number of genetic and lifestyle factors, as well as certain autoimmune disorders, which can increase your risk of DVT, but it most commonly occurs as a result of some type of damage or inflammation of the vein.
What are the signs and symptoms of Venous Thrombosis?
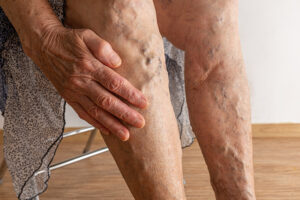
Deep vein thrombosis does not always have noticeable symptoms, but the most common signs include sudden swelling, usually in the legs. There may also be pain or sensitivity in the area, as well as redness or discoloration. The affected area may also feel unusually warm.
What are the risk factors of Deep Vein Thrombosis?
While deep vein thrombosis can affect anyone, there are numerous factors to consider when assessing your level of risk. DVT is more common in adults who are above the age of 60 or who have a close family member who has had issues with deep vein thrombosis in the past. Deep vein thrombosis is also commonly associated with pregnancy/childbirth, recent surgery, or having had an illness or hospitalization which required spending an extended amount of time in bed. There is also a correlation between DVT and some medical conditions including heart failure, inflammatory bowel disease, and some types of cancer.
There are also a number of lifestyle factors which can increase your likelihood of having deep vein thrombosis, many of which are consistent with the risk factors of other cardiovascular issues. Some of these include living a sedentary lifestyle, being overweight or obese, eating an unhealthy diet, or smoking cigarettes. You may also be more susceptible to deep vein thrombosis if you are taking birth control pills or any medication which increases your body’s ability to form blood clots.
How is Venous Thrombosis Diagnosed?
After a review of your symptoms and any relevant family or medical history, your doctor will perform a physical examination of the affected area, checking for swelling, redness, or tenderness. If your doctor suspects that DVT is a likely possibility, there are multiple tests which can be performed to verify the diagnosis. These include MRI, duplex venous ultrasound, venography, or CT scan. Additional tests may also be performed to determine whether an underlying disorder is causing blood clots.
What are possible treatments For Deep Vein Thrombosis?
Venous thrombosis should be treated immediately to minimize the risk of serious complications. Treatment generally revolves around preventing the clot from increasing in size or becoming dislodged and traveling elsewhere in the body through the bloodstream. It is also important to address the root cause of the issue so that further blood clots do not form.
Milder cases of DVT can usually be addressed on an outpatient basis. Anticoagulants (blood thinners) may be prescribed in order to prevent the clot from growing or additional clots from forming. You may also be asked to wear a compression stocking, which facilitates blood flow through the legs and helps to reduce the risk of clotting. For severe cases, thrombolytics (also referred to as clot busters) may be used to break up the blood clot.
If medications are not an option due to side effects, allergic reactions, or other reasons, a filter may be inserted into the large vein known as the vena cava in order to prevent a blood clot from traveling to the lungs.
Are there preventative steps or measures to avoid complications from DVT?
While there is no certain way to avoid deep vein thrombosis, there are several steps that you can take to minimize your risk. Getting regular exercise, eating a healthy diet, and not smoking cigarettes are all crucial to maintaining healthy blood flow. If you spend a lot of time sitting down, such as for a desk job, make sure to stand up and walk around periodically.
If you have had issues with clotting in the past, it’s important to follow any instructions from your physician, including wearing compression stockings and taking any prescribed medications. If you do notice any symptoms such as swelling, pain, or discoloration, it’s critical to report them to a doctor immediately in order to reduce the risk of serious complications.
What are the risks If Deep Vein Thrombosis is left untreated?
The biggest risk that comes with untreated venous thrombosis is a pulmonary embolism, which occurs when the blood clot becomes dislodged and travels through the bloodstream, ending up in the lungs (when this occurs due to DVT, it is referred to as a thromboembolism). This can cause an extremely dangerous blockage of blood flow which can be life-threatening. Symptoms of a pulmonary embolism include dizziness, sweating, severe chest pain, rapid increase in heart rate, and coughing up blood.
Key takeaways about Deep Vein Thrombosis
Venous thrombosis occurs when a blood clot becomes lodged in one of the deep veins, most commonly in the lower legs. It may have no symptoms but can cause swelling, discoloration, and pain in the affected area. This issue can be treated through interventions such as blood thinners and compression socks, with the primary goals of treatment being to keep the blood clot from growing or becoming dislodged and traveling to other parts of the body, and to keep new blood clots from forming. If untreated, DVT can result in a pulmonary embolism, which is very serious and can be fatal. To prevent deep vein thrombosis, it’s important to exercise regularly, eat a nutrient-rich diet, and manage any pre-existing conditions which may impede regular blood flow.



