1 in 20 Americans over the age of 50 has Peripheral Arterial Disease (PAD)
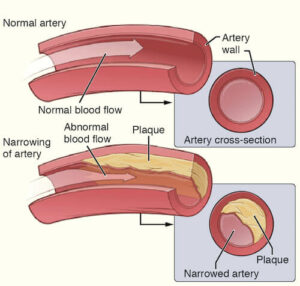 Peripheral arterial disease is a condition that develops when fatty plaque builds up in the arteries and veins of the legs and limits blood flow. Just like clogged arteries in the heart, PAD raises the risk for heart attack and stroke.
Peripheral arterial disease is a condition that develops when fatty plaque builds up in the arteries and veins of the legs and limits blood flow. Just like clogged arteries in the heart, PAD raises the risk for heart attack and stroke.
PAD is similar to coronary artery disease (CAD). Both are caused by atherosclerosis that narrows arteries and blocks proper blood flow to important parts of the body.
What are the symptoms of PAD?
The most common symptoms of PAD in any form include:
- Painful cramping in hip, thigh or calf after walking or climbing stairs
- Leg numbness and a sense of weakness
- Coldness in the lower leg or foot (noticeable on one side)
- Sores on toes, feet, or legs that do not heal
- Change in the skin color of your legs
- Hair loss on legs and feet
- Slower toenail growth
- Erectile dysfunction
It’s important to know that people can have PAD without knowing it. People often experience minor symptoms, such as pain or camping in legs, but don’t report them because they believe they are either a natural part of aging or due to another condition.
But undiagnosed PAD can increase your risk for a coronary artery disease, heart attack, or stroke. If left untreated, PAD can even lead to gangrene and amputation.
What are risk factors for PAD?
The cause of plaque buildup in the limbs is unknown in most cases. However, people who meet one or more of the following criteria may be at higher risk of developing PAD:
- Diabetes
- High blood pressure (or Hypertension)
- High cholesterol
- Smoker or former smoker
- Personal history of vascular disease, heart attack, or stroke
- High levels of homocysteine, a protein that builds and maintains tissue
- Over the age of 50 with a history of diabetes or smoking
- Over the age of 70
Screening for PAD
PAD screening compares the blood pressure in your wrists with the pressure in your ankles using the Ankle-Brachial Index (ABI) and Pulse Volume Recording (PVR). A significant difference between the two measurements may indicate restricted blood flow in the legs from plaque buildup.

During the physical exam, your doctor may feel for your pulse and then get a reading with a blood pressure cuff and ultrasound device. You may also be asked to walk on a treadmill and have readings taken both before and after. If your doctor notices a weak or absent pulse in your leg or foot, or poor wound healing, this may be a sign of PAD.
In some cases, your doctor may even inject a dye into your bloodstream to see how your blood if flowing through your arteries. This dye is detected with X-rays or magnetic resonance angiography (MRA) or computerized tomography (CTA).
If you feel like you or a loved one may be suffering from PAD, don’t wait. Come in for a PAD screening at Manhattan Cardiology. Book your appointment today.

 Peripheral arterial disease is a condition that develops when fatty plaque builds up in the arteries and veins of the legs and limits blood flow. Just like clogged arteries in the heart, PAD raises the
Peripheral arterial disease is a condition that develops when fatty plaque builds up in the arteries and veins of the legs and limits blood flow. Just like clogged arteries in the heart, PAD raises the 

